- What Is a Subconjunctival Haemorrhage Compared to Other Red Eye Conditions?
- Subconjunctival Hemorrhage vs Red Eye: Key Differences
- What Causes Subconjunctival Hemorrhage vs Other Forms of Red Eye?
- How Treatment Differs: Subconjunctival Haemorrhage vs Red Eye Conditions
- When Should You See a Specialist for Red Eye or Subconjunctival Haemorrhage?
- Conclusion
- FAQs
Subconjunctival Haemorrhage vs Red Eye: How to Tell the Difference and When to See a Specialist
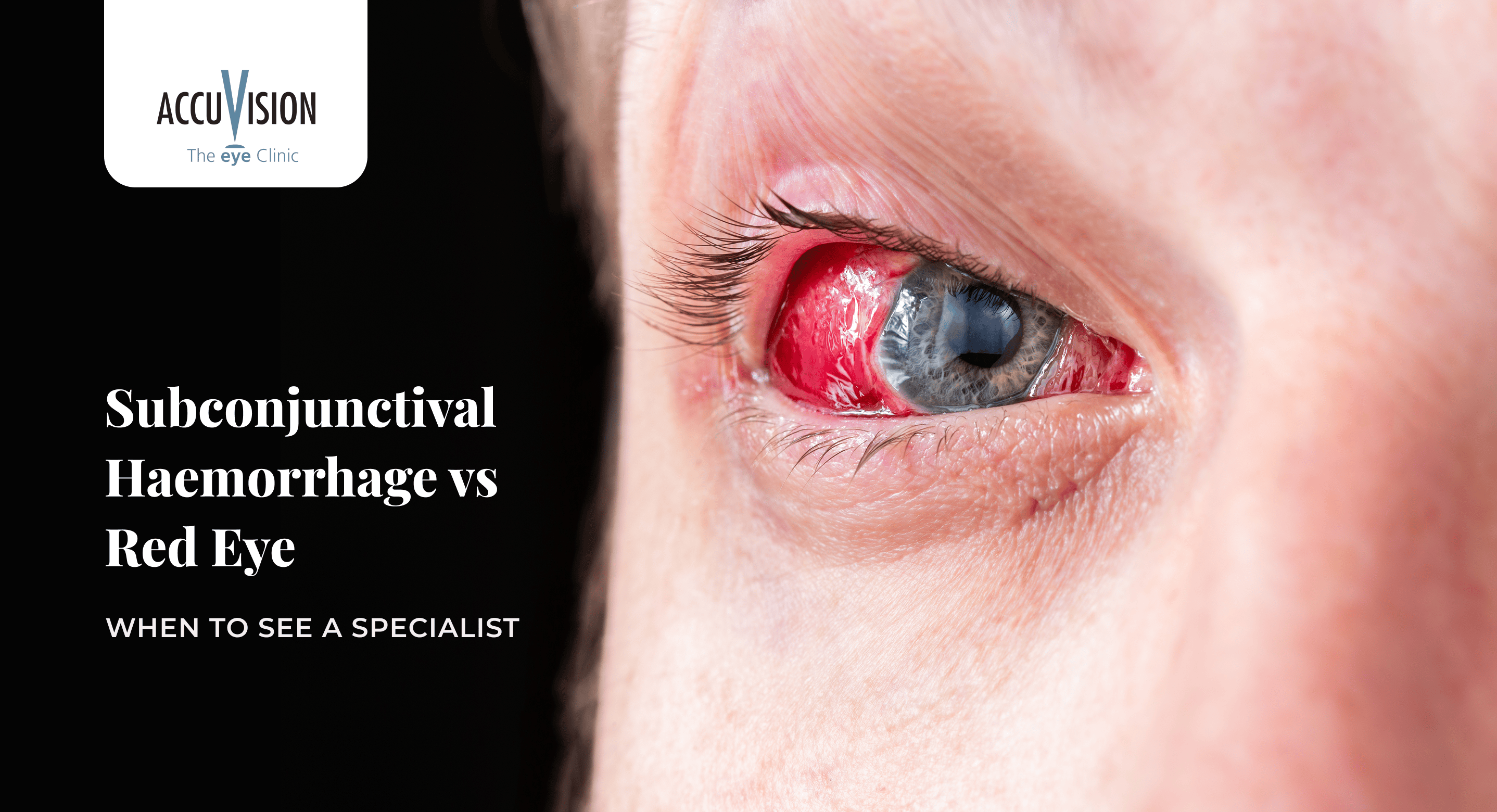
Waking up to discover redness in your eye can be concerning, but not all red eyes signal the same problem. Some people experience diffuse pinkness across the entire eye from allergies or infections, while others notice a dramatic, blood-red patch that appears suddenly overnight.
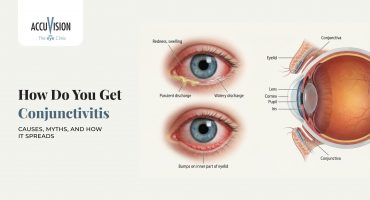
Understanding the difference between subconjunctival haemorrhage and other common causes of red eye is essential for appropriate care. A subconjunctival haemorrhage occurs when a tiny blood vessel breaks beneath the conjunctiva, creating a vivid red patch. In contrast, conditions like conjunctivitis, dry eye syndrome, or uveitis produce different patterns of redness with distinct accompanying symptoms. This guide will help you identify which type of red eye you might be experiencing, understand when the condition is likely to resolve on its own, and recognise warning signs that require specialist attention.
Please note that this article is for general educational purposes only and does not replace professional medical advice. If you have persistent red eye symptoms, pain, or vision changes, a comprehensive eye examination at AccuVision can help identify the cause and guide appropriate care.
What Is a Subconjunctival Haemorrhage Compared to Other Red Eye Conditions?
A subconjunctival hemorrhage occurs when a small blood vessel ruptures beneath the conjunctiva, the transparent membrane covering the white part of your eye. The leaked blood becomes trapped between tissue layers, creating a bright red patch that looks alarming but is typically painless and does not affect vision.
This differs significantly from other red eye conditions. Conjunctivitis, commonly known as pink eye, causes inflammation of the conjunctiva with diffuse redness, discharge, and often a gritty sensation. Dry eye syndrome produces generalised redness with burning and discomfort from insufficient tear production. Uveitis, an inflammation inside the eye, can cause deep redness accompanied by pain and light sensitivity. The subconjunctival haemorrhage stands apart due to its distinctive appearance and absence of pain. While other conditions develop gradually with multiple symptoms, a subconjunctival hemorrhage appears suddenly as an isolated finding.
Subconjunctival Hemorrhage vs Red Eye: Key Differences
Distinguishing between subconjunctival hemorrhage and other forms of red eye requires careful observation of specific characteristics. The following comparison highlights the main differences:
| Feature | Subconjunctival Haemorrhage | Other Red Eye Conditions |
|---|---|---|
| Appearance | Bright red, well-defined patch; looks like blood under clear tissue | Diffuse pink or red across entire eye; bloodshot appearance with visible vessels |
| Pain Level | Usually painless; may feel mild irritation | Often painful, gritty, burning, or aching sensation |
| Discharge | None | Watery, mucous, sticky, or purulent discharge common |
| Vision Changes | Vision remains completely clear | May experience blurred vision, light sensitivity, or visual disturbance |
| Onset | Sudden, often noticed upon waking | Gradual development over hours or days |
| Duration | Resolves naturally in 1-2 weeks | Persists or worsens without treatment |
If you notice a localised, bright-red patch without pain, discharge, or vision changes, you likely have a subconjunctival haemorrhage. However, if redness is accompanied by discomfort, watery or sticky discharge, or visual disturbance, you may be experiencing conjunctivitis, an allergic reaction, dry eye syndrome, or another condition requiring prompt medical attention.
What Causes Subconjunctival Hemorrhage vs Other Forms of Red Eye?
Understanding the underlying subconjunctival hemorrhage causes compared to triggers for other red eye conditions helps clarify which type you may be experiencing.
Subconjunctival Haemorrhage Causes:
These typically involve sudden pressure increases or minor trauma:
- Forceful coughing, sneezing, or vomiting.
- Extremely heavy lifting or straining during exercise.
- Vigorous eye rubbing or minor trauma.
- Blood-thinning medications (aspirin, warfarin).
- High blood pressure, making vessels fragile.
- Spontaneous vessel rupture, especially in older adults.
Common Red Eye Causes (Other Conditions):
These involve inflammation, infection, or irritation:
- Viral or bacterial conjunctivitis (pink eye).
- Allergic reactions to pollen, dust, or pet dander.
- Dry eye syndrome from reduced tear production.
- Environmental irritants (smoke, chlorine, air pollution).
- Contact lens-related irritation or infection.
- Uveitis or other inflammatory eye conditions.
The key distinction is that subconjunctival haemorrhage generally results from bleeding without infection or inflammation, while most other red eye conditions involve inflammatory processes. This fundamental difference explains why treatments vary significantly between the two categories.
How Treatment Differs: Subconjunctival Haemorrhage vs Red Eye Conditions
Subconjunctival haemorrhage treatment differs substantially from managing other red eye conditions, reflecting their distinct underlying causes.
Managing Subconjunctival Haemorrhage:
Most cases require no medical intervention. The blood reabsorbs naturally over one to two weeks, with the red patch gradually fading through various colours like a healing bruise. There is no subconjunctival haemorrhage cure that accelerates this process. Preservative-free artificial tears as advised by your healthcare provider may provide comfort if you experience mild irritation. Cold compresses can soothe the area in the first 24 hours.
Treating Other Red Eye Conditions:
In contrast, other red eye conditions often require active treatment. Bacterial conjunctivitis may need antibiotic eye drops to clear infection. Allergic conjunctivitis can be treated with antihistamine drops and by avoiding known triggers. Dry eye syndrome requires regular care and recommended therapy with artificial tears, warm compresses, and sometimes prescription medications to improve the ocular surface.
Viral conjunctivitis typically resolves on its own but may require supportive care for comfort. Uveitis demands prompt treatment with anti-inflammatory medications to prevent complications. Contact lens wearers with red eyes should immediately discontinue lens wear and seek assessment to rule out serious infections.
The passive approach suitable for subconjunctival haemorrhage would be inappropriate for these conditions, which may worsen without proper intervention. This underscores the importance of accurate diagnosis.
When Should You See a Specialist for Red Eye or Subconjunctival Haemorrhage?
While many cases of red eye and subconjunctival haemorrhage resolve without intervention, certain situations warrant professional evaluation. The urgency differs depending on which condition you’re experiencing.
Seek prompt assessment for subconjunctival haemorrhage if:
- Haemorrhages recur frequently in the same eye or both eyes.
- You are unable to see the border of the red pool of blood.
- The red patch is accompanied by unusual eye pain.
- You experience any vision changes or blurriness.
- The haemorrhage occurred following significant eye trauma.
- Redness persists beyond three weeks with no improvement.
- You notice bleeding or bruising elsewhere on your body.
Seek immediate care for other red eye conditions if you experience:
- Severe eye pain or throbbing discomfort.
- Any changes to vision.
- Extreme light sensitivity that prevents opening your eyes.
- Green or yellow discharge suggesting bacterial infection.
- Red eye following eye injury or chemical exposure.
- Red eyes with headache, nausea, or seeing halos around lights.
- Symptoms that worsen rapidly despite home care.
A comprehensive eye examination can definitively distinguish between subconjunctival haemorrhage and other conditions, assess underlying risk factors such as high blood pressure, and provide tailored management recommendations. Advanced diagnostic equipment allows eye care professionals to examine blood vessel health, measure intraocular pressure, and detect early signs of conditions requiring intervention.
Conclusion
Distinguishing between subconjunctival haemorrhage and other red eye conditions empowers you to respond appropriately when eye redness occurs. A subconjunctival haemorrhage presents as a localised, bright red patch that appears suddenly, causes no pain, produces no discharge, and does not affect vision. It resolves naturally in two weeks without treatment.
Other red eye conditions display different characteristics. Conjunctivitis produces diffuse redness with discharge and discomfort. Dry eyes cause burning and grittiness. Uveitis triggers deep pain and light sensitivity. These conditions require active treatment rather than the watchful waiting appropriate for subconjunctival haemorrhage.
Knowing these distinctions enables you to discern when self-assurance suffices and when seeking professional care becomes necessary. Recurrent subconjunctival haemorrhages, red eyes accompanied by pain or discharge, or any vision changes warrant specialist evaluation.
The experienced team at Accuvision provides comprehensive eye examinations using advanced diagnostic technology to accurately diagnose the cause of your red eye symptoms. Whether you need confirmation about a subconjunctival haemorrhage or assessment of other concerning symptoms, timely professional evaluation ensures appropriate care and peace of mind.
This content was reviewed by the clinical team at AccuVision The Eye Clinic, a trusted UK-based centre for comprehensive laser vision correction and specialised eye care. With expert Ophthalmologists and Optometrists across the UK, AccuVision ensures that every article reflects accurate, medically reviewed information and supports evidence-based eye health awareness. This content is for general educational purposes only and should not be construed as medical advice. Always consult a qualified eye care professional for personalised guidance and treatment of specific conditions.
FAQs
1. How can I tell if my red eye is a subconjunctival haemorrhage or conjunctivitis?
A subconjunctival haemorrhage appears as a bright red patch with no pain or discharge, and vision stays clear. Conjunctivitis usually causes more widespread redness, irritation, discharge, and sometimes blurred vision.
2. How long does subconjunctival haemorrhage take to heal compared to other red eye conditions?
Subconjunctival haemorrhage typically resolves within one to two weeks. Conjunctivitis may resolve within days to two weeks, depending on the cause, while chronic conditions like dry eyes need ongoing care.
3. Can high blood pressure cause both subconjunctival haemorrhages and red eyes?
High blood pressure can increase the risk of subconjunctival haemorrhage by weakening blood vessels. It does not directly cause conjunctivitis, but recurrent haemorrhages should prompt blood pressure checks.
4. Do I need different treatments for subconjunctival haemorrhage versus other red eye conditions?
Yes. Subconjunctival haemorrhage usually needs no treatment. Other red eye conditions require targeted care, such as antibiotics, antihistamines, or lubricating drops, depending on the cause.
5. When is red eye an emergency versus something I can monitor at home?
Painless subconjunctival haemorrhage can be monitored at home. Seek urgent care if redness is accompanied by severe pain, vision changes, discharge, light sensitivity, trauma, or systemic symptoms.